By now you may have heard that NFP, or natural family planning, is more than just avoiding a pregnancy, and it ain’t just for Catholics or married folks. That’s because NFP is nothing more than fertility awareness (FA), a discipline that teaches women to learn to read their fertility, giving them incredible insight into their overall health, and empowering them to pursue holistic health options instead of just hormonal birth control to treat root causes of fertility issues.
The good news is, as a single woman, you’re in the ideal position to learn fertility awareness. You don’t have the pressure of learning a method in the midst of planning a wedding, and family planning is maybe not an immediate concern on your horizon. Maybe you have had some odd things occur in your cycle, like unusual symptoms or mood swings, and you want answers instead of a bandaid in the form of hormonal birth control. Or maybe you are simply tired of being surprised by Aunt Flo.
In my perfect world, all women would be taught fertility awareness at least in some basic form as soon as they start puberty. The benefits are just too great to miss!
So now you’re here – where the heck do you begin?
Disclaimer.
Before I proceed with this post, I need to make very clear that I am not a medical professional nor am I a certified FA instructor. This post is meant purely to give you a starting point so you can understand roughly what fertility awareness does, how to choose a method, and whether to pursue self-teaching for now, or if you would benefit from formal instruction.
I do not promote self-teaching in general. For one, family planning effectiveness statistics for all FA methods include only those women who have received formal instruction. Further, if you are trying to learn your fertility in order to diagnose a fertility issue, you cannot do that through self-teaching. Interpreting and understanding your individual chart and charting your biomarkers accurately requires the aid and guidance of a certified instructor, no matter your chosen method.
However, I do understand that as a single woman, you might not have the time or the funds to make an investment right now, but you would still like to learn more about your body, even to plan simple things like when to throw a tampon or pad into your purse.
This post will hopefully help you navigate all of that.
The Menstrual Cycle.
During one of my OB/GYN appointments, I was asked how long my cycles were. I told the nurse they were on average 35 days long. Her stunned look of horror left me confused, as she asked, “You bleed for 35 days?!” I found myself in the odd position of explaining to a women’s medical professional the difference between a “cycle” and a “period.”
Considering the vast amount of misinformation out there about a woman’s cycle and what’s normal and healthy, I figured I’d start with a basic lesson on the menstrual cycle.
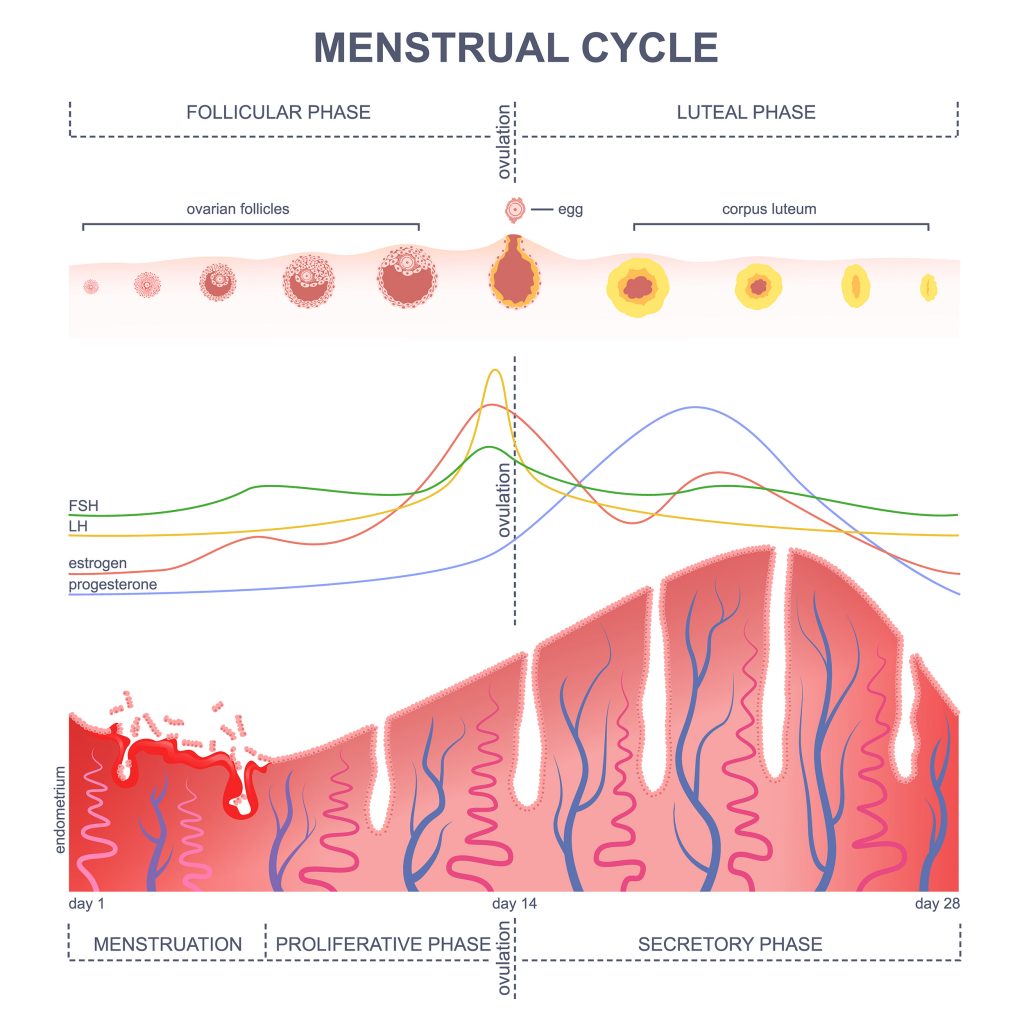
You’ve probably seen some version of this graph at some point in your life, and may have been overwhelmed by what it all meant. That’s ok. Let’s break it down very briefly for our purposes.
Look at the two terms at the top of this graph: the follicular (or pre-ovulatory) phase and the luteal (or post-ovulatory) phase, and the events and hormonal shifts that take place within them.
Now, a healthy cycle isn’t one that is 28 days only. In fact, a healthy cycle can range from 21-42 days, but the average cycle length shouldn’t vary dramatically for an individual woman.
During the follicular (pre-ovulatory) phase, an egg matures in the ovarian follicle (hence the name of the phase), signalled by a rise in estrogen. This rise in estrogen produces cervical mucus, the key external biomarker tracked in fertility awareness. This phase can range in length, and women may note having earlier or later ovulations. Neither is necessarily an indication of an issue in and of itself, unless other unusual symptoms are noted. While the length of this phase can vary woman to woman, a healthy follicular phase shouldn’t change dramatically cycle to cycle for each individual woman (until she enters menopause).
The follicular phase ends when the luteinizing hormone signals the follicle to release the egg, resulting in ovulation. Once ovulation has taken place, the corpus luteum (the leftover follicle) produces progesterone, and the luteal (post-ovulatory) phase begins. Ovulation and the accompanying hormonal shift is most notably marked in the change in basal body temperature, but also in the change of quality of the cervical mucus, followed by dryness. A healthy luteal phase can vary in length between 9-17 days long, while each woman should notice that her individual luteal phase remains fairly consistent cycle to cycle.
Ovulation, not menstruation, is the key event in the menstrual cycle. Ovulation is a sign of health, since the brain and body have to be in sync in order for the symphony of hormones coordinating this event to operate properly. To reiterate, every woman’s cycle length is different, and that cycle length is not in and of itself a sign that something is wrong. Knowing the healthy variations within the follicular and luteal phases helps you understand where your cycle falls on the spectrum of normal, or if it doesn’t, that there may be an underlying issue to address.
*This section was reviewed by a Creighton practitioner.
How Fertility Awareness Works.
All methods of FA are designed to identify the 24-48 hour window when a woman ovulates. Each method of FA will use either one or a combination of biomarkers to identify that window, and a woman learns how to observe and record these biomarkers to give her a picture of her fertility and health.
The biomarkers used to identify this window are: cervical mucus, vaginal sensation, hormone levels, basal body temperature (BBT), and cervical position. These biomarkers change over the course of a menstrual cycle in correspondence with the different hormonal shifts and events illustrated in the menstrual cycle graph.
It’s important to know that there is no such thing as a “best” method of FA. The decision to use one method over another is the result of myriad considerations based on a woman’s state in life, personality, psychological disposition, and other health considerations. I know women who love methods I couldn’t fathom using, and vice versa. The beauty of FA is women have actual choices.
What You Should Consider.
Now that we have that foundation set, here is a short list of things you may want to consider when choosing a method. These questions certainly aren’t exhaustive, and you may think of others to add to the list as you read through them.
- What is my goal with learning FA? Do I simply want a better understanding of my body and moods? Am I trying to identify an issue with my cycle?
- Have I experienced any abnormalities in my cycle, such as painful and/or heavy periods, long (over 42 days) or irregular cycles, irregular bleeding, unexplained weight gain, acne (beyond puberty)?
- Is it a high or low priority for me to be able to discuss my chart with my doctor for the purpose of finding alternative medical treatments?
- What is my lifestyle like? Is my daily schedule fairly regular or more fluid?
- What is my personality? Do I enjoy dissecting detailed information, or do I need my FA method to be fairly simple?
- Am I in a serious relationship discerning marriage? Will family planning be a major concern in the near future?
- What am I able to invest financially? Do I have the resources/need to learn a formal method with an instructor, or do I just need reliable information to learn some basics for now?
A Word on Apps.
Before we get into options after answering those questions, you may be wondering about tracking apps. Some apps claim they can predict ovulation with up to 99% accuracy, and they have FDA approval to boot. Nothing – nothing – can predict or confirm the precise timing of ovulation except daily ultrasounds taken during the fertile window. Any app claiming to predict ovulation is using a computerized form of the rhythm method to do so, not accurately reading your unique chart.
Apps are great for keeping track of your observations, but you should never rely on them to predict ovulation. Some methods do have their own apps like Marquette. Another method, FEMM, is entirely app based, allowing you to connect with an instructor, learn the method, and track your cycle through the app. Other tracking apps I’ve had recommended are Ovia and Clue.
My favorite app for charting is the Read Your Body app. It’s an international non-profit, community-centered app developed exclusively by women who cycle track for women who cycle track. They charge a small annual fee so they can maintain the app and protect user data. It is completely customizable to work with almost every method of fertility awareness, including plugins for technologies like TempDrop. They are constantly updating and improving the app based on user feedback.
When You Want to Learn (but you’re short on time or funds).
So you’ve answered the questions, and you simply want to understand more about how your body works, but you’re still skeptical about the time and monetary investment of learning a whole method.
This list of books was recommended by some fertility awareness users and instructors from my Instagram account. I highly recommend them for anyone, even those who still want to look into formal instruction.
The Fifth Vital Sign
The Art of Natural Family Planning
Garden of Fertility
Natural and Safe: The Handbook
Taking Charge of Your Fertility
Woman Code
When You Want to Take the Plunge (and you need method options).
Now, you answered those questions, and you want to formally learn a method. Maybe there are some health issues you want to address. Maybe you’re a planner and marriage is in your future, and you want to get a jumpstart now. Or maybe all the cool science and gadgets have you totally geeking out, and you want to dive in head first.
Below is a quick run-down of some of your method options pros and cons (not an exhaustive list by any means). Click on each method to access their website so you can learn more about how the method works. *I have also included an instructor list at the end of this post.
Be sure to to check out this series I published earlier this year, Q&As with instructors and users of 5 different methods, so you can compare and contrast real-life situations.
Sympto-hormonal.
- Pros: Utilizes hormone (estrogen and LH) levels only, or a combination of hormone levels, cervical mucus, and basal body temperature (as a user prefers) to identify ovulation. Highly adaptable throughout different fertility stages (ie postpartum). Tend to embrace and research newer tracking technologies to incorporate in the method protocols (ie LH and progesterone strips, Mira monitor, etc).
- Cons: Higher long term costs if using a monitor to track hormones. Windows of fertility may be longer or more difficult to navigate for women with long, irregular cycles, ie PCOS.
- Methods: FEMM, Marquette, Boston Cross Check
Sympto-thermal.
- Pros: Utilizes cervical mucus, basal body temperature (BBT), and cervical position to identify ovulation, increasing user confidence in tracking. Little to no long term costs after initial instruction/ materials purchase. Simple to learn and implement.
- Cons: BBT must be “waking temperature,” taken at the same time each morning within a 30 minute window. Women with varying work schedules (ie nurses) may find TempDrop helpful, but it’s a higher monetary investment. Since BBT only confirms ovulation, it can be difficult to navigate through different fertility stages (ie postpartum, menopause, when ovulation can be indefinitely delayed).
- Methods: CCL, Sensiplan, SymptoPro
Mucus or sensation only.
- Pros: Utilizes mucus or vaginal sensation to identify ovulation. Little to no cost following initial instruction and materials (Billings instructors take donations only). Strongly geared towards identifying and treating root causes of a range of fertility issues (Creighton is used specifically by NaPro certified OB/GYNs).
- Cons: Requires intensive attention to the mucus symptom and sensations. Tracking takes place over the course of the whole day, not just once a day. Tracking other biomarkers is generally discouraged, with exceptions based on a user’s needs.
- Methods: Creighton, Billings
More Questions?
I know that while I covered a lot, you may still have questions, concerns, or need to find community. Make sure to follow me on Instagram where I try to address all of that. I’m constantly sharing information from practitioners and instructors of many FA methods as well as medical doctors, both secular and Catholic, all to help you understand more about the amazing gift that is your fertility.
As I was writing this post, one of my favorite Marquette instructors, Feminine Genius Ministries, announced they would be releasing a course for single women on October 1st. Check out the details below, and click the image to visit their website

An introductory course that covers all of the important components for female charting— and leaves out the family planning details.
It will explain how to track mucus, how to do urine hormone testing, and how to track temperature. There will also be an overview of charting red flags, mood characteristics of the follicular and luteal phases, and wellness suggestions to maintain optimal cycle regularity and overall health.
Charting template included for paper charts or customizable online spreadsheet charting.
+
$25 for the online course.
Follow up purchased separately, if needed.
*Below is a list of some of my favorite instructors from various methods.
Marquette.
You, Me and NFP/ Sarah Tramonte, RN
Feminine Genius Ministries (several instructors)
Sara Flood, BSN, RN
Whole Mission/ Theresa Sullivan, RN
Creighton.
Mary Bruno, CRMS
Lisa Morvant, RN, BSN, FCP
Fertility Coaching and Wellness/ Holly Baril, CFCP
Charbel Centre, Canada/ Rebecca McEvoy, MSc, FCP
Billings.
Leslie Rewis MA, MLIS
NFP Aware/ Kristin Putnam
Boston Cross Check.
Christina Valenzuela (Currently not taking clients, but still an excellent resource for understanding BCC)
FEMM.
Celine Kinneberg, RN
Cassondra Moriarty
Sophia/ Sage Fertility
Sympto-Thermal.







Leave a comment